Blog
Can Hypopressives Help Diastasis Recti?
Continuing my education as a core fitness specialist is crucial to me, and my goal is at least 30 hours every two years. In May, 2019 I was able to attend the first Low Pressure Fitness Level 1 Certification to be held in the United States. The 2-day, 16-hour workshop was led by Dr. Tamara Rial, and I was one of only two fit pros while the rest were physical therapists. My main reason for gaining understanding and experience in this exercise technique was to ascertain if hypopressives can help diastasis recti. Overall, my hypothesis is that — done correctly — this style of low pressure fitness is a great abs exercise for abdominal separation.

So how might hypopressives help diastasis rectus abdominus?
During the training, we got to see two ultrasounds done in real time. One was on Dr. Tamara as she performed various hypopressives in supine, kneeling, and all-fours positions. She did not have diastasis, and her linea alba held strong with every breath-hold (apnea). Then a course participant with a mild diastasis offered to be scanned. Her diastasis was only 2.5-3 fingers, which I would call borderline, and her linea alba widened slightly BUT thickened substantially during the hypopressive action.
As I have discussed here and here on Fit2B, we have to include the chemistry and tension necessary to stimulate fibroblasts to lay down new connective tissue — the process of restoring the abdominal wall. Hypopressives not only clearly reverse outward pressure on the linea alba, they also stimulate the muscles and fascia as discussed in this article.

Hypopressives = Negative Pressure
Therapy for diastasis rectus abdominus typically involves great attention to the management of intra-abdominal pressure (IAP) and avoiding motions that create excessive outward bulging of the midline down the center of the abs. Hypopressives literally do the opposite, pulling the abs inward and upward into a concave shape. So, should we be worried about this “reverse” pressure?
If it’s not good for the abs to be pressured very far outward or forward, how is it good for them to be pressured inward? What happens to the pelvic organs during a hypopressive?
The unique thing about this type of ab work is that it’s not a conscious “abdominal drawing in maneuver.” In the image above, I’m not pulling my navel to my spine on purpose by engaging my transverse abdominis. It looks like I’m sucking in my breath and holding my chest up, but I’m not.
The inward motion of the abs happens at the base of an exhale which is held for an average of 5-10 seconds while the ribs are purposefully opened wide, using the diaphragm, intercostals, and latissimus.
Some call it a false inspiration. Except, if you try to inhale without actually breathing in — like, if you plug your nose and close your mouth while trying to draw in air — your abs will likely pull in, and your ribs will flare out, but you’re not technically doing a hypopressive. Rather, you’re doing something closer to what’s known as the Mueller Technique. If you close your airway completely and hold your breath on an inhale, that’s called a valsalva maneuver. A proper hypopressive feels very similar to Uddiyanha Bandha to me.
I believe Hypopressives help Diastasis
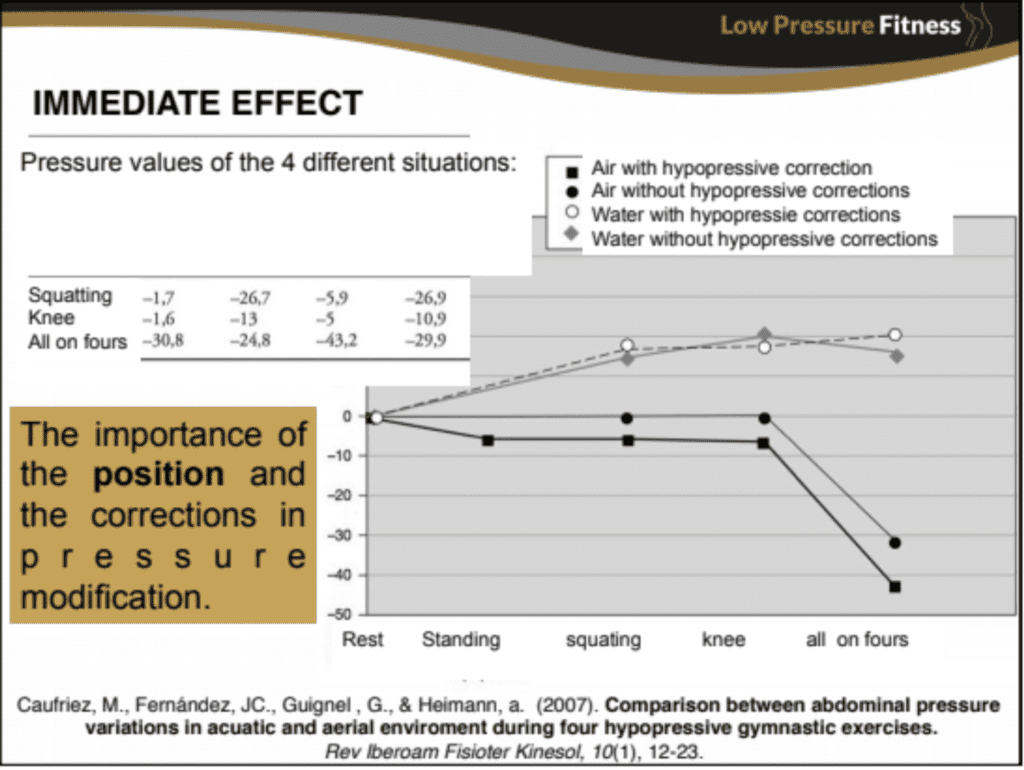
As you can see from the chart which I’ve linked to Dr. Tamara’s website, pressure in the core went DOWN more when hypopressives were used on land compared to water! Usually people get into the water to reduce pressure. What if it could be reduced without getting into a swimsuit and getting wet? The results my clients are getting from using hypopressives to help with their Diastasis are huge!
Two studies that caught my attention
One of the issues I face with my clients is that transverse abdominis (TA) incorporation is pivotal to core training and diastasis healing, but there’s a tendency to over-squeeze. The “go big or go home” mentality is hard to fight in the fitness industry, and teaching “lighter not tighter” and “consistency beats intensity” pits me against a natural tendency toward “all or nothing.” However, if the transverse gets squeezed too tight, it easily shifts into bearing down which then creates outward bulging pressure on the muscles supporting the bladder, colon, and uterus.
A 2011 study by Stüpp compared abdominal hypos with pelvic floor muscle exercises, looking at the effect of TA contraction in 34 subjects (physical therapists, none of which had given birth before, and more than half of which were physically active). They found that hypos produced less TA contraction than PFM exercises, but when the two exercises were combined there was better contraction than pelvic floor muscle exercise alone.
In 2012 Resende & Bernardes et al studied a cross sectional area of levator ani in 58 women with stage II pelvic organ prolapse and compared pelvic floor muscle training with hypopressive exercises. The women were put into 3 groups: normal pelvic floor exercises, hypopressive exercises, and a control group. Similar increases in the cross sectional area of levator ani produced with both pelvic floor exercises and hypopressive exercises were reported. Also, both types of exercise improved pelvic floor function, but adding hypopressives to pelvic floor exercises did not yield further improvement compared to pelvic floor exercise alone.
My deductions from those two studies are that hypopressives are a valuable tool for people who tend to over-flex their transverse abs. Indeed, as I have added hypopressives to the Fit2B workout library and my in person training sessions, I have witness how, if someone isn’t connecting to regular pelvic floor exercises and cues then hypos truly improve their symptoms!
We did a podcast about hypopressives and diastasis with one of my faves
The Fit2B Radio podcast is available on iTunes and all other podcasting platforms, and I’ll do a happy dance if you subscribe. However, you really should catch the video version of this episode here because it shows me doing my FIRST ever “hypo” which is the nickname for these highly detailed exercises. Kim trained directly under Dr. Tamara’s co-founder. She had to allow me to cheat with a little “Mueller” nose-plugging to help me feel it the first times. I’ve since learned to do hypopressives without cheating.

Learning Hypopressive Poses
That picture of me practicing my hypos at home in my mismatched pajamas just a week after official training became my baseline photo. This style of core training was initially really challenging for me, and maybe that’s why I’ve enjoyed it so much. It has taken my brain and body (as well as my clients’) in a whole new direction, and I’m learning another set of words to express abdominal ability.
Since completing training, I spent 6 months practicing on individuals and small groups before filming two basic hypopressive video workouts for Fit2B entitled Ebony Exhale and Cobalt Core. The first routine, Ebony Exhale is part of our Black Color Series of workouts, and it is all the Level One poses, minus the apnea or vacuum. This enables people to learn the proper positioning of the arms, torso, and feet. Then the second routine, Cobalt Core, is part of our Blue Color Series of workouts with the apnea layered in along with a couple new poses.
Can Hypopressive Videos Work?
While cuing hypopressives to help Diastasis Recti via video isn’t generally recommended, many people don’t live near a certified hypopressive instructor like myself, nor can they afford to pay $20 or more per class, let alone pay for a private session. Fit2B offers hundreds of high quality home workouts, including hypopressive video routines, for the cost of a few fancy coffees per month!
In our pro-quality home exercise videos, you’ll find something for every mood, time frame, fitness style, and ability level. We also offer highly specialized routines for various chronic life conditions.

After completing my training with Dr. Tamara, I spent almost a year honing my cues in class settings and private sessions. Learning which verbiage got the best response within a class of 10 or more enabled me to design the hypropressive workout videos we have here on Fit2B and know that people will have success.
As the founder of Fit2B, I’m always available in my private member forum to answer questions, and I also offer online consultations for people who want and need individualized programming beyond my professionally filmed home workout videos. I truly love what I do and love helping people put the puzzle of their core together.
Can Hypos Hurt You?
Any exercise has the potential to cause harm. Not all exercises are suitable for all bodies. Timing also plays a huge role in deciding if a certain exercise is right for you.

Contraindications include pregnancy, high blood pressure, IUDs, heart disease, pulmonary diseases, anxiety, stomach illness or inflammation, or surgery less than 3 months ago.
What do you think about hypopressives?
Have you had the chance to try them? Did you learn alone or were you trained by someone? If you have diastasis and you’ve tried them, do you think they have helped or not? Have hypropressives helped your pelvic floor muscle function? I’m so curious to learn more about this method and start a research project with Dr. Tamara soon! I’ll keep you posted!